
Yes. My left knee. And the mighty muscle groups of my thundering hams (att. G. Ainsworth), visible in this new (to me) form of imaging.
The knee is the largest and most complex joint in the body. As is customary when finding out more than skin deep things about the body, the correct response is to reel back in awe. Not a simple hinge, its components glide and roll about on each other.
 The posterior and anterior cruciate ligaments are key elements holding it together. Appearing in pink in the middle of this simplified illustration, they are ‘cruciate’ because they are arranged like an ‘X’, a cross. The medial ligament at right here protects against excessive lateral movement. They can all be torn from their moorings or ruptured. Ruptured ACL? 9 months after surgery before you’re going again.
The posterior and anterior cruciate ligaments are key elements holding it together. Appearing in pink in the middle of this simplified illustration, they are ‘cruciate’ because they are arranged like an ‘X’, a cross. The medial ligament at right here protects against excessive lateral movement. They can all be torn from their moorings or ruptured. Ruptured ACL? 9 months after surgery before you’re going again.
Knees are the body’s shock absorbers. The load exerted on each knee joint during walking is three times body weight (bang 240kgs, bang 240kgs, etc and that’s just strolling along), climbing stairs about four times, squatting more than five. Cycling interestingly is only 1.2. Swimming too is lower because of the supported nature (bike seat, water) of each activity.
The major cushioning apparatus is visible in the digram above as well. The two ‘disks’ made out of fibrous cartilage are the medial and lateral menisci. They protect the ends of the bones from rubbing on each other and effectively deepen the sockets into which the femur, the thigh bone, attaches. They play a role in shock absorption, and when the knee is forcefully rotated and/or bent, can be cracked or torn.
The white material on the end of each bone represents hyaline cartilage preventing bone from ever rubbing on bone. Many times smoother than Teflon, the smoothest artificial substance ever produced, this form of cartilage — most unusually — lives without a blood supply and therefore can’t heal itself. Once it has formed in childhood, the cells hardly grow or develop further. Wear and tear is irreversible. If the cartilage is cracked, torn, or worn through, the bone of the joint itself will suffer. We call that osteoarthritis. Bone grinds on bone. Inflammation and pain result.
* * * * * *
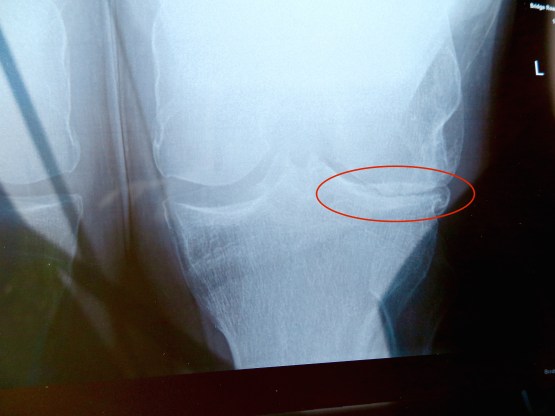
Does that look it needs a replacement? I asked the radiologist. Mmmm, she said nodding sagely, not much daylight there.
I have had trouble with my knees since my early teens. ‘Long-jumping into hard pits’ was one causative diagnosis. Sore knees stopped me playing football for what I like to think would have been the pinnacle of my glory days. I had my first (of three) athroscopies of the knee more than 30 years ago. (Arthroscopies: key hole surgery of the knee to tidy up tears in the cartilage surface and remove floating pieces, now widely discredited in terms of impact and usefulness.) An osteopath looking through my history recently found the first reference to knee pain in 1991. Lately, coming down mountains, not going up so much, the grind of bone on bone is so tangible that I imagine I can hear it, and sometimes I can.
However. However. However.
Have you had any trouble washing and drying yourself because of your knee? How much has pain from your knee interfered with your usual work? (including housework)? Could you do household shopping on your own? Could you walk down a flight of stairs? I even struggled with, How would you describe the pain you usually have in your knee? (It’s not regular. It comes and goes. Sometimes it hurts. A lot. But you know … )
These are questions from the Oxford Knee Score to assess what sort of intervention you might need with graded multiple choice answers. Answering best and as honestly as I could I scored 42, the interpretive key for which was ‘Mate piss off. There’s nothing wrong with you. Step out of the way for people who actually need help.’ And you go along to the surgeon’s rooms and are sitting with mostly men, just as it happens, who are knotted up with arthritis, need help standing and then get along, just, with a stick.
An imposter perhaps?
Eighteen months ago I had a discussion with a knee surgeon who happened to be Irish, who pointed to what the right questions for me were. Eighteen months later I went to see him again and talked about lying awake at night with pain, beginning to drag my left leg consistently, and taking far too many anti-inflammatories which were beginning not to work. I seemed to have made up my mind and he didn’t dissuade me.
One salient issue is just how long the artificial joint might last. If the answer is 15 years and you’re 55, you might want to think about that. But if the answer is probably 20 years, as it seems to be at present, and you’re nearly 70, well …
So I washed myself down with chlorhexidine, told forty people serially what my name and date of birth were, and de-suited up.
* * * * * *
“I regard the theatre as the greatest of all art forms, the most immediate way in which a human being can share with another the sense of what it is to be a human being.”
— Oscar Wilde
 This quote, although intended to reflect on the performing arts, also quite aptly defines the goings on in a surgical operating theatre. The term ‘Theatre’ conjures images of live drama and suspense. It is a rather appropriate and symbolic idiom. Historically, the first operating rooms were amphitheatres in which the surgeon, dressed in street clothes, performed operations on a raised table or stage, surrounded by several rows of students and other spectators who could observe the case in progress. Needless to say, this was by no means a sterile environment but the spectacle was certainly captivating.
This quote, although intended to reflect on the performing arts, also quite aptly defines the goings on in a surgical operating theatre. The term ‘Theatre’ conjures images of live drama and suspense. It is a rather appropriate and symbolic idiom. Historically, the first operating rooms were amphitheatres in which the surgeon, dressed in street clothes, performed operations on a raised table or stage, surrounded by several rows of students and other spectators who could observe the case in progress. Needless to say, this was by no means a sterile environment but the spectacle was certainly captivating.
Brian Devitt, my Irish surgeon, to the left above, wrote and shared this.
The structure of the operating room has evolved over time. In reality, the amphitheatre no longer exists, having been replaced by smaller, less populated, and cleaner rooms. Nevertheless, the symbolism continues. There is a still a well-established routine. The actors (surgeons) are adorned in distinctive costumes (scrubs, gowns, and gloves) for the show. Next, the patient, the main character in the production, is wheeled into the room for the performance with prodigious ceremony, assuming centre stage under the spotlights to join the awaiting cast (scrub nurses and junior doctors) for the main act.
The operating room is a surreal place with countless rules, which are policed by the ever-vigilant theatre sister. As a medical student this is one of the most foreboding venues one must venture during rotations. With so much going on, you are always in someone’s way, despite trying to conceal oneself, chameleon-like, against the walls: ‘Don’t touch this. Don’t stand there. Keep your hands in. Stop breathing.’ Life is less ominous as a doctor when there is a specific role to play. In a junior capacity, the doctor is often the whipping boy, suffering a baptism of fire in this high-pressure setting. Although, with added experience and seniority, the now surgeon assumes a greater leadership role within the team.
The theatre is generally a very calm environment. Most cases are routine and have a set procedure. The most hectic period is at the beginning of the case when the anaesthetized patient is wheeled into the operating room on a trolley and transferred to the operating table for surgery. Orthopaedic surgeries normally require a very specific set-up, and in some cases a specialized system of traction is employed to facilitate the reduction of a fracture. Following this, the surgical site is painted with antiseptic solution and isolated with sterile drapes. What follows next is probably one of the most simple, yet effective advances in reducing surgical complications in recent times; the surgical time out. Everyone stops. A checklist is read out, detailing the procedure, highlighting that the correct side has been marked, and ensuring the necessary equipment is available and appropriate antibiotics have been given. Finally, surgery can begin.
To watch a gifted surgeon operate is like watching Riverdance. Every step, each movement is choreographed and purposeful. The surgeon speeds up during routine dissections and debridement [removal of damaged tissue], but slows down when making critical decisions and approaching vital structures.
Each team member should be synchronized to facilitate the surgeon. As is often said facetiously, the assistant’s job is to make the surgeon look good. There’s generally not much room for conversation during a case. Commands are given clearly and succinctly. The scrub nurse is a crucial team member, supplying the correct instruments swiftly, safely and ergonomically to the waiting surgeon. In many cases an experienced nurse will know what the surgeon needs before he asks. The eponymously named instruments can be confusing, particularly to the junior surgeon. An exhortation is often heard to ‘give me what I want, not what I ask for.’
Thankfully, in most cases the final scene of these endeavours finds a healthy, happy patient. Life in theatre is tough and tiring but very rewarding. Once the final curtain has been drawn, sleep is not difficult to find. That sleep is deep, restful and well earned.
* * * * * *
I asked the physician consulting on my case if they cut the bone out or if it was just resurfacing. These questions… you don’t even now what you’re asking half the time. He stifled a roar of laughter and indicated that yes the bone would most certainly be cut out. Not only that, but it would hurt like buggery.
This is one absolutely consistent theme of people who I have spoken to about knee replacements. The one area of absolute agreement among participants, qualified professionals, relatives, onlookers, grocers who have met someone once whose cousin … is the degree of pain, described by my consulting physician as ’10 times worse than a badly-sprained ankle (or, in technical terms, 10xb-sa). … And it doesn’t stop!’ he amplified. ‘Not immediately anyway.’
So I woke up in an opioid-induced haze. Not asleep yet not quite awake, and unsure if those cows I was chasing were real ones, and if they were what I needed to do about it. These are the glories of Targin, a mixture of oxycodone and naloxone. Oxycodone is a narcotic pain reliever and naloxone belongs to a group of medications known as opiate antagonists used to lessen the constipation caused by oxycodone. But in case that doesn’t work, and it doesn’t appear to, there are regular doses of Coloxyl and other incentives to internal movement.
How was I feeling? Fine. Great. I got out of bed — a cautious and controlled swing of the new one, it could have fallen off — and tested it on the floor. In terms of stability (and feel) it felt remarkably like it did before. And boy, did I get told off. In my defence, I did this because I was making an extra effort to urinate. I ate and drank and watched a series of television programs which wandered in and out of my conscious reality.
The next day I walked 647 steps — I know that because I had my phone in my pocket — and tackled the stairs down to the coffee shop. The nurses began calling me One Day David.
The second morning was the only time it really hurt, but even then maybe only 2.6b-sa or even less. A second chemical weapon was employed which blasted this problem to smithereens.
* * * * * *

Now here I am eight days later sitting at home blogging away and uncertain about tone management.
It’s going well. Can I say that? Just nice and flat? Going well. Last night it hurt but I’ve been off everything but Panadol (and anti-inflammatories and blood thinners — no one’s taking any chances here) for a few days, and I have this visual metaphor of the knee unfreezing — it remains quite swollen — and exposing the actuality of what is under the ice. Pain in this case means not being able to find a comfortable rest point. Wherever you put the leg, you need to move it again immediately to try something else. There will be a name for that.
That’s on the one hand. On the other I walked up to see my GP today — I suppose that’s about a kilometre — and going up and down stairs is no problem. In fact I’m back to normal pattern (one step, next step, next step, not one step one step, next step next step) for going up and am close for going down. I’m not doing my physio in an orderly way because I think I’m getting quite lot of incidental exercise, and while walking is easy there are certain lifting actions that feel like a horizontal incision is being ripped apart with the terrible mental presentiment that that is actually what is happening. I tend to avoid actions like that. And any lateral pressure. There is some disorder in any recovery.
Three months they say before walking is as normal, another few weeks before I can drive a car. In the meantime I have no trouble getting to Trutrack for a coffee fix.
So. Good I guess. But not triumphalist. I’m not running down the road to the gym yet, and I’ll be sitting round quite long enough to have me chafing. But yeah. Good I guess. Good. That just about covers it.
And mightily grateful for just how skilled these clever, kind and thoughtful people who advised, operated on and nursed me were.

I feel for you, David. You have taken your readers right into the middle of things, surgery-wise. I was grimacing slightly at the thought of being one small step away from such an injury to need an operation, but thankful that my knees allow me to do whatever until that moment.
Although I am currently a “one voltaren a week” man, I will need your surgeon’s name sooner or later. And I admire you for all that walking you did recently! How I cant imagine. Well done Bunky.
Your comments about what is inside the knee made me think that I never really want to have anything done to it. Yesterday I played golf for the first time since November and I’m suffering today. Your comment that you can never find a comfortable position is true for me at the moment. I went to my wonderful physio today and he gave me some exercises that will fix things up eventually. My recovery is nothing like yours will be and this too puts me off doing anything about my knees.
Norman Swan should be worried and while my knee appears fine currently, Brian looks right up my alley should I need his support.
All quite fascinating. Amazing how you can be so dispassionate about your experiences. Now if it were me, it would have sook written all over it. But then again it probably wouldn’t get written for the same reason. Whereas this is interesting! Glad you are progressing reasonably well, though reading between lines – not easy. Thinking of you.
All very interesting. You write about it all with such a dispassionate eye. Now if it were me it would have ‘sook’ written all over it. Then again it probably wouldn’t get written for the same reason. I guess you need to be able to hover above your experience to make it interesting to others. I hope it gets easier for you, cos it sounds a bit tough though you’re not saying that. J
As always your blog is informative and entertaining. I feel very fortunate in having sturdy trouble-free knees, at least so far. You’ve got me wondering about the loads exerted on knees during Mitzi’s gloriously knee bending dance moves. How does dancing compare with walking for such things? And I wish you an ever decreasing xb-sa score
Thanks David
Another good read.
And a great way to help fill the two hour wait at Roms gymnastics!
Let’s hope you’re fully recovered in time for your next (walking) holiday. I have to admit I looked away from some of the photos and the video – I’d never have made a doctor (or a nurse). Get well soon.
Pingback: Blog 99 | mcraeblog